Slipped Disc vs Herniated Disc: What Fishers Patients Should Know
Slipped disc vs herniated disc usually describes the same general issue in everyday conversation. “Slipped disc” is the common term, while “herniated disc” is the more accurate medical term for when inner disc material pushes through or against the outer layer and may irritate a nearby nerve. The disc does not literally slip out of place, and not every disc problem causes symptoms.
For many people in Fishers, IN, the real question is not which term sounds worse. The real question is what the disc is doing, whether a nerve is involved, and what kind of care makes sense for the symptoms you have right now. A proper evaluation is important because a sore low back, pain down the leg, numbness, or weakness can come from several different causes, not only a disc issue.
Slipped disc vs herniated disc: are they actually different?
In plain English, most people use slipped disc, herniated disc, ruptured disc, and sometimes even slip disk in back to mean a disc problem that may be irritating a nerve. In clinical language, though, herniated disc is the more precise term. That matters because a bulging disc is not always the same as a herniated disc, and a painful nerve symptom pattern is not always caused by a disc at all.
A helpful way to think about it is this:
| Term | What people usually mean | Why it matters |
|---|---|---|
| Slipped disc | A general, non-medical term for a disc problem | Useful in conversation, but not very specific |
| Herniated disc | Inner disc material pushes outward and may affect a nerve | More medically accurate and often used on exams or imaging |
| Bulging disc | Disc extends outward but may not tear or press on a nerve | May or may not cause symptoms |
| Pinched nerve | A nerve is irritated or compressed | Can be caused by a disc, but also by other spine problems |
When patients hear different words from friends, urgent care, or online articles, they often assume they are being told different diagnoses. In many cases, they are hearing different labels for the same general problem. What matters most is your symptom pattern, your movement limits, your nerve findings, and whether the symptoms are improving or progressing.
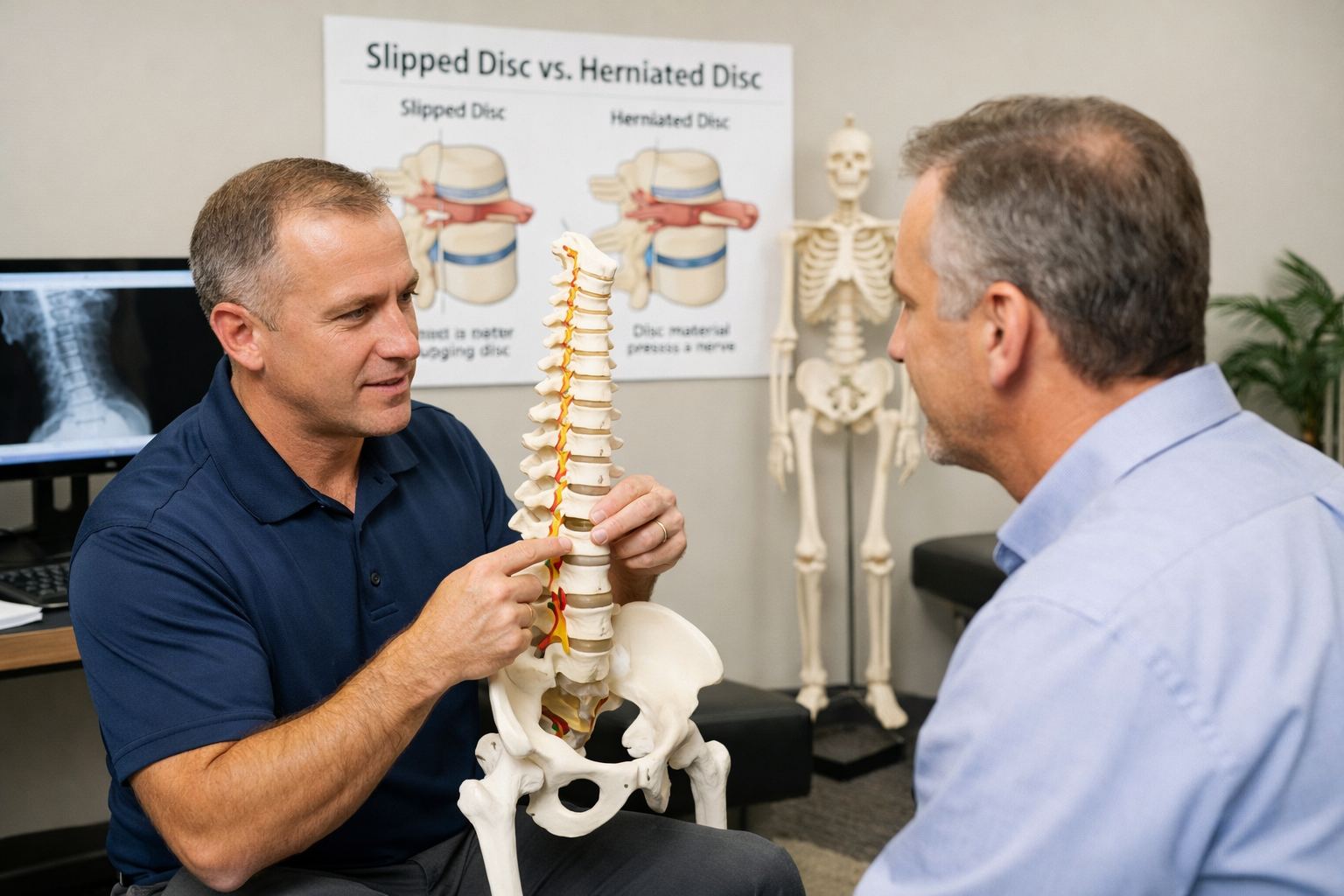 What a herniated disc lower back problem can feel like
What a herniated disc lower back problem can feel like
A herniated disc lower back issue often causes more than simple soreness. Some people feel sharp or burning pain into the buttock or leg. Others notice tingling, numbness, or weakness. Sitting for long periods, bending forward, coughing, or lifting can make symptoms worse for some patients. Still, some disc changes show up on imaging even when a person has little or no pain.
Common symptoms may include:
- Low back pain
- Pain that travels into the buttock, thigh, calf, or foot
- Numbness or tingling
- Muscle weakness
- Trouble standing fully upright
- Increased pain after prolonged sitting
- Symptoms that shift with certain movements or positions
This is one reason self-diagnosis can be tricky. A strained muscle, irritated facet joint, sacroiliac irritation, spinal stenosis, spondylolisthesis, or other causes of radicular pain can feel similar at first. If you want a deeper breakdown of symptom clues, our article on how do I know if I have slipped a disc can help you understand what providers usually look for during an exam.
It is also important to watch for red flags. New loss of bowel or bladder control, numbness in the saddle area, or rapidly worsening leg weakness can signal a medical emergency and should be evaluated right away.
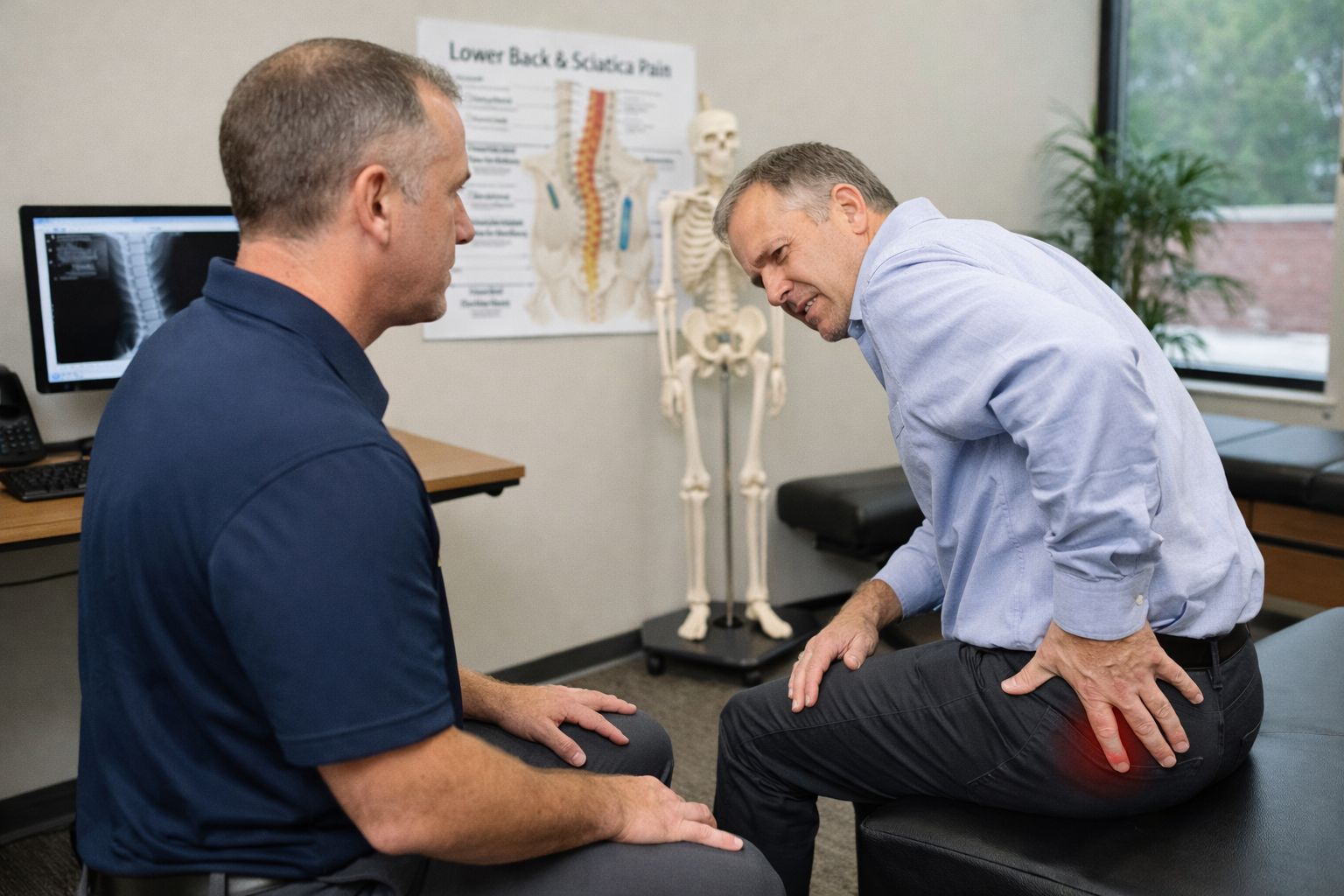
 How providers tell whether symptoms are coming from a disc
How providers tell whether symptoms are coming from a disc
A provider does not diagnose a disc issue by pain alone. The exam usually starts with your symptom history. Where is the pain? Does it stay in the back or travel down the leg? Is there numbness, tingling, or weakness? What movements make it worse? Are symptoms getting better, staying the same, or progressing?
From there, an evaluation may include:
- Posture and movement testing
- Orthopedic tests that help reproduce or ease symptoms
- Reflex checks
- Strength testing
- Sensation testing
- Walking and balance observation
- Checking whether certain positions centralize or spread symptoms
Imaging is not always the first step. Many cases improve with conservative care, and MRI is often more useful when symptoms are severe, persistent, or linked to significant neurological changes or red flags.
At Vital Connection Chiropractic, the goal is not to chase labels. It is to understand whether your presentation looks mechanical, neurological, inflammatory, or mixed, and then decide whether conservative care is appropriate, whether co-management is needed, or whether the safest next step is referral.
Slipped disc vs herniated disc treatment: what usually helps first
For most people, early care focuses on reducing irritation, protecting function, and avoiding the cycle of pain, stiffness, and deconditioning. Disc symptoms often improve over time, especially when care is matched to the person, the severity, and the stage of recovery. The right plan often depends on whether pain is staying local or traveling, whether weakness is present, and how long symptoms have been going on.
Conservative care may include:
- Relative rest instead of full bed rest
- Short, frequent walks
- Temporary activity modification
- Ice or heat depending on what feels better
- Guided movement and mobility work
- Position changes throughout the day
- Supportive strategies for sitting, lifting, and sleeping
- Individualized chiropractic care when appropriate
- Collaboration with other providers when imaging, medication, or specialist referral is needed
If pain control is one of your biggest concerns, you can also review our pages on pain reliever for slipped disc and slipped disc for more context on common symptom patterns and conservative next steps.
| Situation | What may help | When to get checked sooner |
|---|---|---|
| Mild to moderate pain without major weakness | Gentle walking, position changes, relative rest, guided care | If pain keeps spreading or is not improving |
| Pain with tingling or numbness | Conservative care plus an exam to check nerve involvement | If numbness worsens or affects daily function |
| Pain with clear leg weakness | Prompt professional evaluation | If weakness is progressing |
| Severe pain with bowel, bladder, or saddle symptoms | Emergency evaluation | Go to the ER immediately |
One mistake many people make is staying in bed too long. Too much inactivity can lead to more stiffness and weakness, while smart movement can support recovery. The goal is not to “push through” strong symptoms. The goal is to keep moving in a way your body tolerates.
 Is walking good for a slipped disc?
Is walking good for a slipped disc?
In many cases, yes. Gentle walking is often better than complete rest because it keeps the body from becoming more stiff and deconditioned. Short walks can also be easier to tolerate than long sitting sessions. That said, walking should be adjusted to your current symptoms. If a five minute walk feels okay but a twenty minute walk flares your leg pain, that shorter amount may be the better starting point.
A few practical walking tips for Fishers patients:
- Start with a short distance that does not clearly worsen symptoms.
- Keep your stride relaxed.
- Avoid carrying heavy bags during early flare-ups.
- Stop and reset if leg pain starts traveling farther down.
- Break activity into several short walks instead of one long session.
- Pair walking with posture changes during desk work or commuting.
If walking sharply increases numbness, weakness, or radiating pain, that is a sign to scale back and get evaluated. “Good soreness” and clear nerve aggravation are not the same thing.
 How do you fix a slipped disc?
How do you fix a slipped disc?
There is not one universal fix because the best approach depends on the severity of the herniation, whether a nerve is involved, how irritable the symptoms are, and whether there are red flags. Many people improve with conservative care. A smaller group needs imaging, medication support, injections, or surgical consultation if symptoms do not improve or neurological deficits worsen. Surgery such as discectomy is usually considered when nonsurgical care is not enough or when urgent neurological issues are present.
In a chiropractic setting, care may focus on movement assessment, symptom behavior, joint and soft tissue function, posture, exercise guidance, and treatment modifications based on tolerance. Individualized care matters. A person with mainly localized back pain may need a different plan than someone with strong leg symptoms or significant weakness.
For many adults in Fishers, the most helpful first step is not guessing. It is getting a proper evaluation, learning what movements help versus irritate the area, and using a plan that can be adjusted as symptoms change.
Is a slipped disc worse than a herniated disc?
Usually, no. In everyday conversation they often mean the same thing, so one term is not automatically worse than the other. Severity is better judged by function and findings, not by the label alone. A person with mild back pain and no nerve deficit may have a far less serious problem than someone with progressing leg weakness, even if both say they have a “slipped disc.”
That is why clear communication matters. Patients often become more anxious when they hear multiple terms. In reality, what matters most is whether there is nerve irritation, how severe it is, how long it has lasted, and whether symptoms are improving with conservative care.
When to seek urgent care or emergency help
Most disc flare-ups are not emergencies, but some situations should not wait. Seek urgent or emergency care if you have:
- New bowel or bladder control changes
- Saddle numbness
- Rapidly worsening leg weakness
- Severe symptoms after major trauma
- Pain with significant fever or other concerning whole-body symptoms
- Symptoms that are suddenly much more severe and disabling than before
These situations may point to something more serious than a routine flare-up and deserve immediate medical attention.
What this means for patients in Fishers, IN
If you are searching online for “slipped disc chiropractor near me,” it usually means you want two things fast: a clearer idea of what is going on and a practical plan for what to do next. At Vital Connection Chiropractic, the focus is on understanding whether your symptoms fit a disc pattern, what may be aggravating it, and whether conservative care makes sense for you.
For some patients, the next step is improving movement tolerance and reducing nerve irritation. For others, the next step is imaging or referral. Either way, getting checked can help you stop guessing and start making better decisions about work, exercise, sleep positions, and daily activity.
If you are dealing with back pain, leg pain, or numbness in Fishers, IN, the safest approach is a careful exam and a plan built around your presentation, not just the label. When you are ready, you can schedule appointment with Vital Connection Chiropractic to discuss the next best step.
FAQ
Is a slipped disc worse than a herniated disc?
Usually no. In most everyday use, slipped disc and herniated disc mean the same general problem. What matters more is whether symptoms are mild and improving or whether there is strong nerve irritation, weakness, or emergency red flags.
Can a slipped disc heal itself?
Many disc-related flare-ups improve over time with conservative care, activity modification, and guided rehab. Healing timelines vary, and a proper evaluation is important if symptoms are intense, persistent, or getting worse.
How do you know if your disc is slipped or herniated?
Most people cannot confirm that at home with certainty. A provider looks at symptom history, movement testing, nerve findings, and sometimes imaging. The terms are often used interchangeably, but the exam helps determine how involved the disc and nearby nerve may be.
How do you fix a slipped disc?
Treatment often starts conservatively with relative rest, walking, posture changes, symptom-guided exercise, and other non-surgical care. Some people also need medication support, imaging, injections, or surgical referral depending on the severity and progression.
Is walking good for a slipped disc?
Often yes, as long as it is gentle and does not clearly worsen radiating symptoms. Short, tolerable walks are usually better than prolonged bed rest, but the amount should match your current symptom level.


 How providers tell whether symptoms are coming from a disc
How providers tell whether symptoms are coming from a disc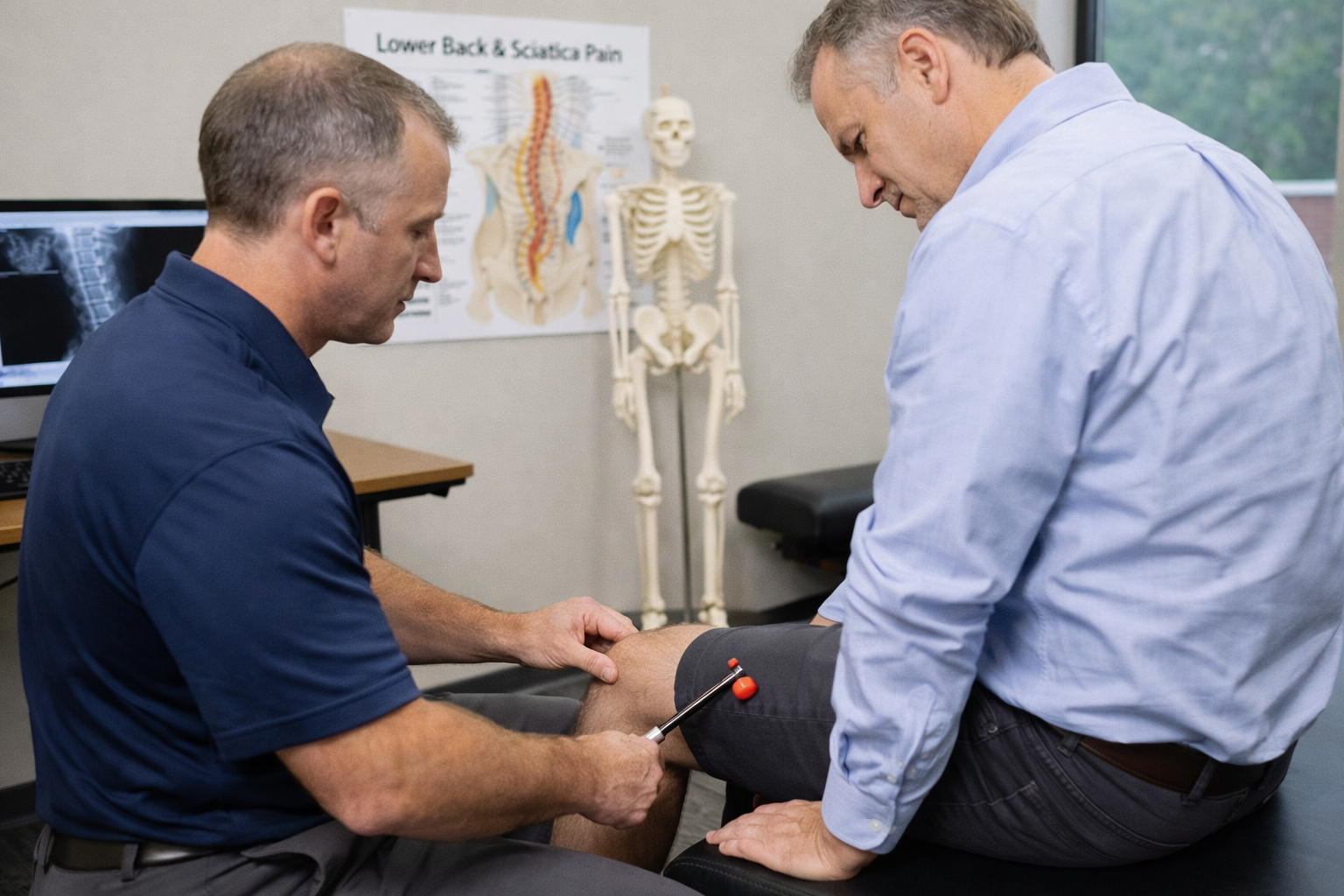 Is walking good for a slipped disc?
Is walking good for a slipped disc? How do you fix a slipped disc?
How do you fix a slipped disc?


